Breathwork for PTSD: What to Know
Trauma does not only live in memory, it lives in the body. For many people navigating PTSD, the nervous system remains on high alert or, at times, completely shut down. Breathwork has gained attention as a supportive tool for trauma recovery because the breath sits at the intersection of body and mind. In this article, we explore how breathwork can be a supportive practice for people navigating PTSD.
What Is PTSD?
Post-traumatic stress disorder (PTSD) is a psychiatric condition that can develop after someone has experienced or witnessed one or more deeply distressing or life-threatening events, such as serious accidents, natural disasters, violence, abuse, war, or medical trauma.
For many people, initial reactions to trauma are intense but often diminish over time; with PTSD, however, symptoms such as intrusive memories, heightened stress responses, avoidance of reminders, or emotional numbing persist for more than one month and begin to interfere with daily life, relationships, and well-being.
Importantly, PTSD is not just psychological - it is physiological. Trauma reshapes how the nervous system functions. After overwhelming stress, the body’s survival response can become chronically activated, keeping the sympathetic nervous system in a prolonged state of “fight or flight,” even when danger is no longer present.
The “fight or flight” condition can look like a racing heart, shallow or rapid breathing, muscle tension, and constant hypervigilance. At the same time, the parasympathetic nervous system which is responsible for rest, digestion, and recovery, may have difficulty activating, making it hard for the body to return to a felt sense of safety.
These nervous system changes also affect brain regions involved in fear, memory, and emotional regulation, helping to explain why people with PTSD may experience reactivity, avoidance, dissociation, and difficulty settling both physically and emotionally.
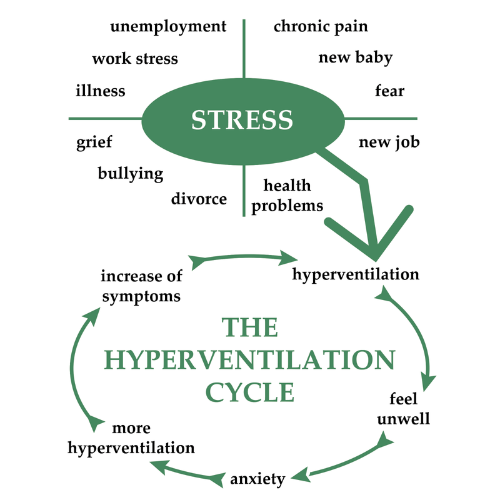
How Trauma Affects the Breath
Source: Calm Clinic
Trauma dysregulates the autonomic nervous system - The part of the nervous system that regulates body functions automatically, without conscious control, such as breathing, heart rate, and digestion, which directly shapes how we breathe. When the body is stuck in a survival response, the breath often becomes shallow, rapid, held, or restricted.
In states of hyperventilation, breathing tends to move into the upper chest - quick, tight, and effortful, as the sympathetic nervous system prepares for threat. In contrast, during dissociation or shutdown, the breath may become faint, barely noticeable, or subtly paused, reflecting a protective withdrawal from overwhelming sensation.
The breath is not malfunctioning in these moments; it is adapting. It mirrors the body’s survival strategies. In this way, our breathing patterns tell the story of what our nervous system has endured, and how it learned to cope.
Also Read:How to Calm the Nervous System with Breath
Can Breathwork Help PTSD?
To regulate the nervous system, breathwork can support people living with PTSD, but not all breathwork practices are appropriate for trauma. Because PTSD affects the autonomic nervous system, working directly with the breath can gently influence that system.
Slow, rhythmic breathing, particularly with a slightly longer exhale has been shown to stimulate the parasympathetic nervous system via the vagus nerve, increasing vagal tone and supporting the body’s capacity to shift out of chronic “fight or flight”. Over time, this can improve nervous system regulation, reduce baseline anxiety, and create more access to a felt sense of safety.
Trauma-informed breathwork can also help rebuild body awareness in gradual, titrated ways. For those who experience dissociation, mindful breathing can become a bridge back into the body. Not by forcing intensity, but by strengthening the capacity to stay present with sensation. However, it’s important to be clear: breathwork is not a replacement for psychotherapy, medical care, or comprehensive trauma treatment. It is a supportive modality; one that works best alongside therapeutic support, not instead of it.
Dangers of Breathwork for PTSD
While breathwork can be supportive for trauma recovery, it is important to acknowledge the risks, especially within an increasingly unregulated breathwork industry. The rapid rise in popularity of breathwork has led to many practitioners offering trauma-related sessions without sufficient training in nervous system regulation, trauma psychology, or crisis management. When working with PTSD, this lack of regulation and trauma-informed understanding can cause significant harm.
For example, some first-time sessions are structured as long, highly intense experiences and marketed as “trauma release.” For someone with PTSD, this approach can be destabilizing. The nervous system may already be operating in survival mode, and pushing it into heightened activation without adequate preparation can increase symptoms rather than relieve them.
An intense breathwork session without proper grounding and integration can leave a participant feeling emotionally raw and physiologically dysregulated. Instead of promoting healing, it may amplify hypervigilance, emotional reactivity, anxiety, or difficulty settling which are core symptoms of PTSD. Without careful pacing and support, the body can interpret the intensity as another threat.
Additionally, deep breathing techniques can surface buried memories, sensations, or emotions very quickly. If a facilitator lacks the training to recognize trauma responses or safely contain intense reactions, the participant may feel overwhelmed, unsupported, or retraumatized. This can reinforce feelings of unsafety in the body rather than rebuild trust.
A single negative experience can also discourage someone from exploring breathwork again, potentially closing the door to a modality that could have been helpful. For individuals with PTSD, breathwork must be approached with clinical awareness, ethical responsibility, and a strong foundation in trauma-informed care.
What Trauma-Informed Breathwork Looks Like
Trauma-informed breathwork is not about pushing intensity or chasing catharsis. It is choice-based, meaning participants are continually reminded that they are in control of their pace, depth, and level of engagement. Nothing is forced. Participants are taught skills that allows them to create a sense of safety in their bodies, so that they can manage the intensity of their breathwork experience.
Here are the principles of Trauma-Informed Breathwork
Safety and Consent: The foundation is establishing a secure space where participants retain full autonomy, with the freedom to pause, adjust, or stop the practice at any point.
Gradual, Gentle Pacing (Titration): Rather than using intense or fast breathing techniques, the practice starts softly and increases only when the participant feels ready, preventing overwhelm to the nervous system.
Emphasis on the Exhale: To help settle the fight-or-flight response, practices prioritize slow, extended exhalations that support calming the sympathetic nervous system.
Grounding and Stabilization: Sessions include grounding practices both before and after breathwork to help participants stay oriented, present, and regulated.
Non-Judgmental Environment: All emotional, physical, or energetic responses are welcomed and validated. Nothing is forced, and experiences are met with compassion rather than criticism.
Importantly, trauma-informed breathwork prioritizes resourcing over release. Instead of trying to “break through” defenses, it strengthens internal stability - cultivating sensations of grounding, support, and capacity.
Also Read: Why Trauma-Informed Training Matters in Breathwork
Gentle Breath Practices for PTSD
When living with PTSD, the goal of breathwork is not intensity - it is safety and steadiness. These gentle practices can help support nervous system regulation. Move slowly, and if at any point you feel overwhelmed, dizzy, emotionally flooded, or unsafe, stop and return to normal breathing. You are always in control.
4–7–8 Breathing:
In this method, you inhale for four counts, hold for seven, and exhale slowly for eight. Repeating this sequence several times encourages relaxation and helps bring awareness to both the breath and bodily sensations.
Conscious Connected Breathing:
Conscious connected breathing involves a continuous flow of breath, with no pause between the inhale and exhale. The breath is full and connected, often directed into the lower belly. This creates a steady rhythm that builds intensity over time.
High Ventilation Breathing:
This more activating technique uses faster, forceful breathing to help release stored tension. Begin seated or lying down. Inhale deeply through the nose, then exhale strongly through the mouth with an audible “ha” sound. Continue at a quicker pace for three minutes. Because of its intensity, this method should be approached with care.
Box Breathing:
This technique follows a steady rhythm: inhale for four counts, hold for four, exhale for four, and hold again for four. Repeat this cycle for several minutes while paying close attention to the sensation of breathing. The structured pattern can promote a deep sense of calm, similar to the relaxation experienced in yoga or meditation.
Deep Belly Breathing (Diaphragmatic Breathing):
Sit or lie comfortably with one hand on your chest and the other on your abdomen. Inhale deeply through your nose so that your belly expands while your chest remains relatively still. Pause briefly, then exhale slowly through your mouth, feeling the belly soften. Continue for several minutes, focusing on the movement of the abdomen and the rhythm of the breath.
Sighing Breath:
In a comfortable seated or standing position, take a deep inhale through the nose, filling the belly. Hold briefly, then release a long, audible sigh through the mouth. Repeat several times, allowing the body to gradually unwind and soften.
These practices are meant to build capacity gradually. If you have severe symptoms, a history of panic with breathing exercises, or complex trauma, consider working with a trauma-informed professional who can guide you safely.
Breathwork can be a powerful companion in the healing process, but it is not a shortcut or a substitute for comprehensive trauma care. The breath is most supportive when approached with gentleness, choice, and respect for the body’s pace. For some, simple practices like slow exhalations or diaphragmatic breathing may be enough to begin restoring regulation. More intensive techniques should always be explored with proper guidance.
If you are seeking a structured and trauma-informed space to explore this work more deeply, we run breathwork courses twice a year, please see our courses above. If you are interested in training to become a breathwork facilitator, click here to request a brochure and we will be in touch with more information.